Skin Imperfections
Of all the other skin growths you can develop, cysts and skin tags are among the most common. These features often start out small and localized, and many people do not at first realize that they have them. While they are usually benign, they can sometimes threaten your health or quality of life. We are thus happy to offer inspections and treatments for both.
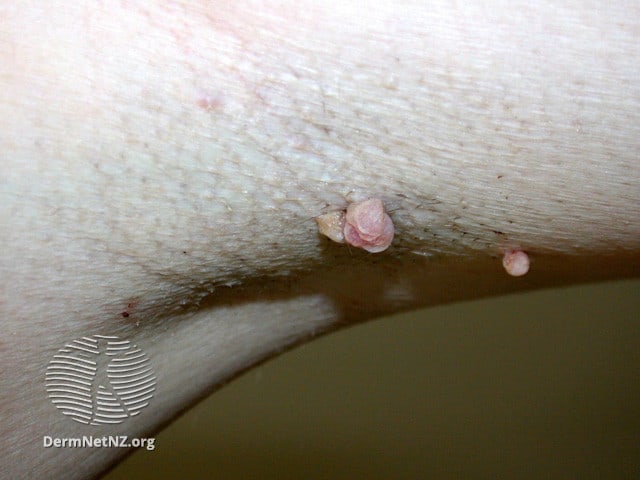
Skin Tags
They tend to develop in areas where bits of skin rub together on a regular basis, such as under the armpits, beneath the breasts, on the underarms, above and beneath the eyelids, and in the intersection between the thighs and the groin. They are not dangerous and shouldn’t be painful. But they can be unsightly and may cause discomfort. Tags can develop on people of any age or health background, but they are particularly likely to affect adults who are overweight. Genetics also appears to play a role; if your parents or close relatives have these growths, you are likely to get them as well.
While there is little that you can do to prevent skin tags, they are relatively easy to remove. While these growths are not cancerous and generally present little to no direct health risk, many people still choose to get them removed for:
- Cosmetic Concerns – Some people do not like the look of skin tags, especially if they develop in visible areas. Because removing them carries few risks, it is perfectly acceptable to have them treated for cosmetic reasons alone.
- Pain Prevention – If skin tags come into contact with jewelry or harsh clothing, they can become irritated and painful. Removing them is the most reliable way to protect yourself from this pain.
- Impeding Infection – Skin tags that regularly become irritated can eventually break open, causing them to bleed and raising the risk of infection. While this is a low risk, many patients choose to eliminate the danger entirely through safe, professional removal.
While skin tags themselves are not cancerous, they are sometimes hard to distinguish from other types of growths that can be. The only way to know for certain that they do not create a cancer risk is to examine some of them in a laboratory and make sure they are skin tags. In addition, tags can sometimes be the result of acromegaly, polycystic ovary syndrome, and other hormonal issues that can themselves put your health at risk. Thus despite the generally benign nature of these growths, we recommend that you let us take a look at them if you develop them in large numbers.
When you have skin tags removed, it is crucial that you let qualified medical professionals do the job. If you attempt to remove them on your own, not only are you less likely to succeed, but you also raise the risk of infection. Instead of taking this risk, let us provide quick, effective skin tag removal. We offer a variety of different options to get rid of these growths, including:
- Surgical Removal – The simplest way to eliminate skin tags is to surgically cut them off. This has the benefit of getting rid of them immediately. It does, however, raise the risk of bleeding or local infection, though we can keep these risks under control by sterilizing the area during the procedure and giving you instructions to enhance healing after treatment.
- Liquid Nitrogen – As an alternative to surgery, we can freeze your skin tags with liquid nitrogen. While this does not get rid of them immediately, they should fall off shortly after the procedure. This method does not carry a risk of bleeding or infection, though it can lead to temporary discoloration in the area that we treat. You may also need additional treatments if the tags do not all fall off after the first round.
- Electrocauterization – Besides freezing, we can also get the tags to fall off by applying a mild electric current. We use a Hyfrecator that applies the least amount of heat possible to safely and effectively eliminate skin tags while leaving the rest of the skin unaffected. This has many of the same advantages and disadvantages as freezing; it does not lead to infection, but may discolor your skin and doesn’t always work the first time.
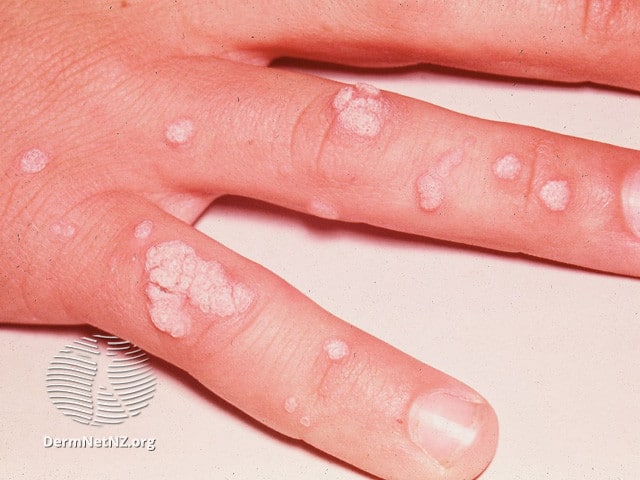
Warts
They have a rough texture and can appear smooth, similar to a blister, or with hard bumps, similar to cauliflower. They may also have black dots as a result of tiny blood clots. There are multiple types of warts depending on where they are on the body:
- Verruca vulgaris – common warts
- Verruca plana – flat warts
- Plantar warts – warts on the bottom of your feet
- Condyloma acuminatum – genital warts
It is important to have your warts evaluated by a dermatology provider as they can also be more dangerous lesions in disguise such as squamous cell carcinoma. Treatment options include:
- Liquid Nitrogen – We can freeze warts with liquid nitrogen. While this does not get rid of them immediately, they should fall off shortly after the procedure. This method does not carry a risk of bleeding or infection, though it can lead to temporary discoloration in the area that we treat. You may also need additional treatments if the wart does not all fall off after the first round.
- Prescription Creams – Immune response modifiers may be used to treat genital warts that are outside of the body. However, it is not a cure for genital warts and may not prevent spreading the virus to others. New warts may also continue to develop. For best results, follow instructions exactly as prescribed by your provider.
- Salicylic Acid – Salicylic acid is applied consistently at home to chemically exfoliate and remove the skin cells until the wart is gone. With continued daily application, the wart will be removed over the course of several weeks.
- Surgical Removal – If the wart is very large or in a difficult place to treat with a different method, we can surgically cut out the wart and close it with stitches. It does, however, raise the risk of bleeding or local infection, though we can keep these risks under control by sterilizing the area during the procedure and giving you instructions to enhance healing after treatment.
Cysts
They can occur anywhere on your body, including your scalp, but are most likely to appear on your neck, trunk, or face. Skin cysts usually start out small and grow slowly, which is why many people who have them do not notice for long periods of time. They are typically painless but can become painful if they are ruptured or infected.
As with skin tags, your risk of developing cysts is partially determined by genetics. In particular, some genetic diseases make cysts significantly more likely, those these disorders are relatively rare. In addition, cysts are more likely to develop in areas of your skin that you have injured. They become more likely after you go through puberty.
Whereas skin tags themselves are not cancerous, cysts can be, which is why we recommend letting us inspect any cysts that you develop. Besides skin cancer, cysts also increase your risk of:
- Infection – Cysts that are ruptured can quickly become infected. When this happens, a boil will develop on your skin, which must be treated as quickly as possible.
- Inflammation – Irritated or ruptured cysts are often subject to heavy inflammation even when they do not become infected. Inflamed cysts are usually tender and heavily swollen; it is often not possible to treat them until the swelling has subsided.
- Chronic Pain – Though cysts are usually painless, if they become irritated or inflamed, they can cause you serious discomfort. For the sake of your quality of life, it makes sense to remove them.
No matter how large or painful your cyst is, you should resist the urge to pop or pick at it, as this can make the problem worse and lead to a higher risk of infection. Instead, schedule an appointment with us to have the cyst removed. You have a myriad of options to get rid of cysts safely and with minimal discomfort, including:
- Medication – One way to reduce the size and swelling of cysts is to inject a medicine that lowers inflammation. This may not completely eliminate the cyst, but it should make it easier to live with and prevent some of the associated risks.
- Drainage – The simplest way to scale back a cyst is to cut a minor incision with a sterilized scalpel. We will then gently remove the keratin inside. This method allows us to quickly reduce the size and impact of the cyst, but it does not get rid of it or prevent it from eventually returning to its full size. Since cysts do not disappear on their own, this means you will likely need repeated treatments over time.
- Surgery – The most reliable way to get rid of cysts is to remove them surgically. After providing the necessary sterilization and anesthetic, we will cut the cyst away and stitch up the wound; you will then have to return to get the stitches removed. Surgery gets rid of the cyst for good, and it is perfectly safe. We cannot perform it, however, on cysts that are inflamed, so you may have to undergo one of the other treatments or wait for the swelling to go down before we can get started.
Whether you decide not to remove a cyst or are waiting for the swelling to go down, you can keep inflammation under control by applying a warm, wet cloth to the area. This helps the cyst to drain and makes you less likely to develop scars or infections. You should also avoid squeezing or picking at the cyst. We are happy to provide you with advice on proper cyst care before, after, or as an alternative to removal. By giving you the knowledge for effective cyst management as well as offering professional treatments at your disposal, we leave you prepared for every variety of skin growth.
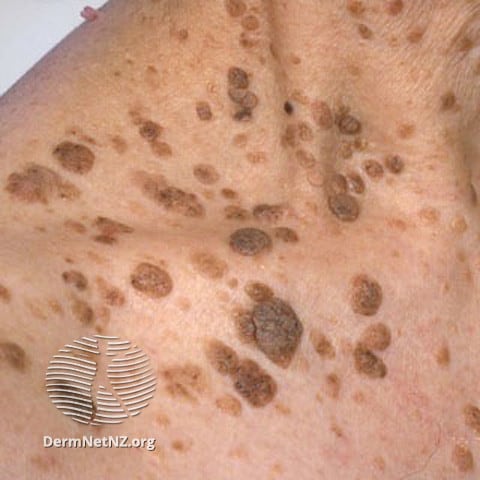
Seborrheic Keratosis
This light brown, black or tan growth may be slightly raised from the skin surface and have a “crocodile” scale or shiny appearance. These spots aren’t contagious or painful, and they aren’t thought to be caused by sun exposure as one might think. They seem to run in families so if your mother or father had them, you may develop this condition. Some people may experience itching, which may lead to scratching and bleeding.
While they aren’t necessarily dangerous, they can be very unsightly, spanning as much as an inch in diameter and often developing in clusters. Fortunately, you don’t have to live with Seborrheic Keratosis. You have treatment options:
- Liquid Nitrogen – We can freeze your seborrheic keratosis with liquid nitrogen. While this does not get rid of them immediately, they should fall off shortly after the procedure. This method does not carry a risk of bleeding or infection, though it can lead to temporary discoloration in the area that we treat. You may also need additional treatments if the SK does not all fall off after the first round.
- Electrocauterization – We use a Hyfrecator that applies the least amount of heat possible to safely and effectively target Seborrheic Keratosis with just the right amount of heat, removing keratosis without harming deeper or surrounding tissues. Generally, removal results in normal-looking skin after healing has taken place. The treatment takes around 30 minutes, and recovery time is typically one to six weeks, depending on the lesion size and other factors that could slow healing.
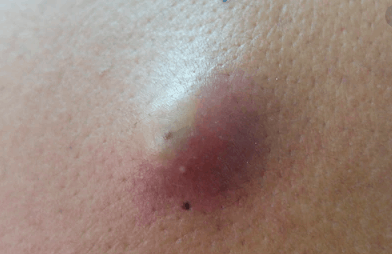
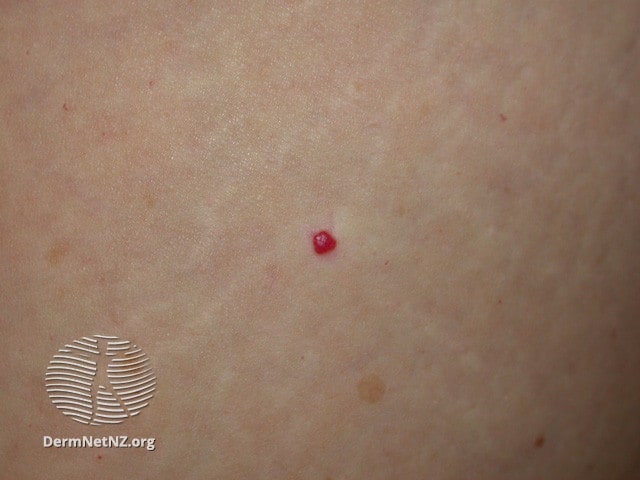
Cherry Angiomas
Alternative names for them include “senile angiomas” and “Campbell de Morgan spots”. They receive their characteristic reddish color from the fact that very small blood vessels come together in that area. The cause is unknown.
Cherry angiomas are typically not a health concern unless they bleed randomly or experience changes in shape, size or color, which indicate possible skin cancer. But they can be unsightly. Many people choose to have them removed and you have a great option should you choose to do so.
Cherry angiomas are treated with:
- Electrocauterization – We use a Hyfrecator, a minimally-powered medical device, to very precisely target the cherry angiomas, destroying the tissue safely while preventing excess bleeding. The treatment takes approximately 30 minutes and the treated area heals in as little as one week.
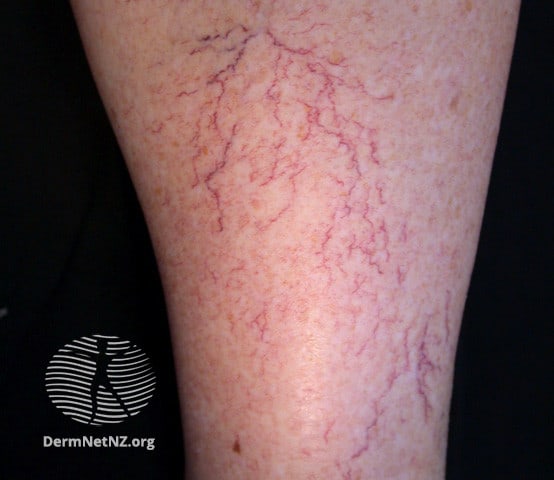
Telangectasias (Spider Veins)
Telangectasia is the technical name for spider veins, clusters of dilated capillaries visible under the skin that may resemble a spider’s legs or web. An estimated 50% of adults have spider veins. They’re typically the result of excessive sun exposure or significant pressure to the surface of the skin, which causes vessels to burst. Prolonged sitting and crossing the legs apply this pressure so it may increase your risk, but spider veins aren’t necessarily a sign of a sedentary lifestyle. They run in families and are very easy to develop.
Unless accompanied by severe varicose veins, they’re not generally dangerous, but they are very unsightly and many people choose to have them removed. For those people, there are some very effective treatments for spider veins:
- Electrocauterization – We use a Hyfrecator to very carefully target the spider veins without damaging surrounding tissues. The procedures typically take around 30 minutes with a recovery time of about one week, during which you can continue normal activities.
- Laser treatment – BroadBand Light laser can heat and eliminate these fine vessels. BBL is a comfortable and quick treatment that will give rather quick results. Your skin will be cleansed and protective eyewear will be placed over your eyes. A cool gel will be applied to the treatment area. The proper filter and setting will be chosen for your specific needs. During the treatment, most patients say it feels warm and similar to that of a quick rubber band snap. It takes about 20 minutes from start to finish.
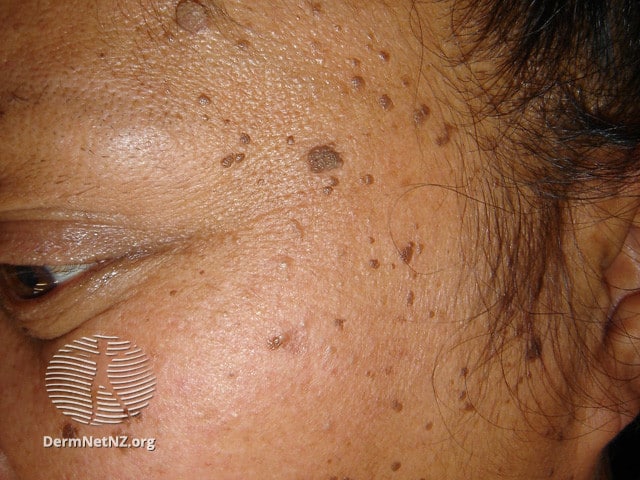
Dermatosis Papulosa Nigra (DPN)
DPN is characterized by the presence of many, small, smooth, hard, dark brown or black lesions that can be up to 5mm (nearly 1/4 inch) in diameter. They’re common in people of color. Approximately 35% of African-Americans have them and dark-skinned people of Asian descent are at higher risk of developing these aesthetic imperfections, although the exact prevalence in this group is unknown.
Those who develop Dermatosis Papulosa Nigra, typically see their first dermatoses in their teens, but as they age the number increases and can “take over” the face or other parts of the body. The medical community believes that DPN has a strong genetic component, and may occur because of genetic variation related to hair follicles.
- Electrocauterization – We use a Hyfrecator to precisely target DPN, in order to create a smoother and more even-looking appearance. This procedure is typically not recommended for people who develop keloid scarring or are likely to suffer from hyper-pigmentation or loss of pigmentation as they may be unable to achieve an even appearance.